Design-Based Reduction of Catheter-Related Bloodstream Infections
Team Members: Supada Sritanyaratana, Kenneth Gao, Albert Lin, Homayun Mehrabani
Capstone Client: Hobart Harris, MD, MPH, Professor and Chief, Division of General Surgery at UCSF
Purpose:
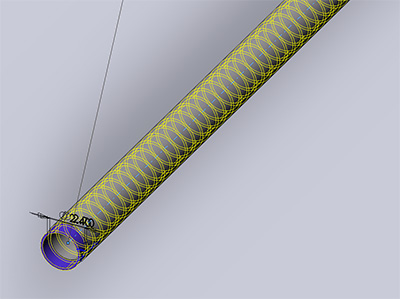
Microbial growth and infection of central venous catheters can lead to catheter-related bloodstream infections (CRBSIs) causing 28,000 deaths and a medical cost of $2.3 billion in the U.S.A. annually. Bacterial biofilms formed on the surfaces of catheters act as reservoirs for pathogens by resisting traditional antimicrobial methods. Protection of catheters from bacterial biofilms can reduce the occurrence of CRBSIs. Our team decided to pursue an electrified catheter concept to inhibit biofilm formation due to the presence of electric fields in the catheter. In our design, electrically isolated conductive bands inside the catheter’s wall create electric fields from band-to-band, inhibiting biofilm formation near the catheter walls.
Imaging of mouse model retinas
Team Members: Robert Chen, Shayan Fakurnejad, Ha Sung (Leo) Moon, Kimberly Chan
Capstone Client: Michael Ward, MD, PhD, Resident Physician of Neurology at UCSF; Ari Green, MD, Assistant Professor of Clinical Neurology at UCSF
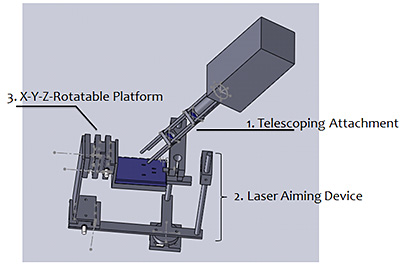
Purpose: One method to diagnose and monitor the progression of neurodegenerative diseases in mice models is the imaging of the retina by a scanning laser ophthalmoscope (SLO). However, SLO systems designed for humans need to be adapted to function optimally with mice. A lack of appropriate restraint systems and imaging procedures for use with mice result in suboptimal retinal images and can result in corneal clouding. To solve these problems, our team developed a restraint system for high resolution movement of an SLO about the fixed point of a mouse retina, a telescoping lens attachment, and a laser alignment system to adapt an SLO for use with mice.
Enabling a Laparoscopic Imaging Device to Overcome the Need for Continual Clean Up
Team Members: Nasim Barzanian, Neil Ray, Sakthivel Nagaraj, Jeffrey Yang
Capstone Client: Joe Forrester, MD, MSc, Stanford University Department of Surgery
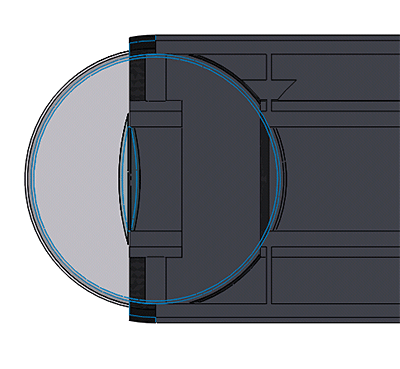
Purpose: Laparoscopic surgery relies on an unobstructed view of the inside of the body through the laparoscope camera. Currently, when the camera is obstructed by fog, bodily fluids, or stray tissue, the surgeon must stop surgery and remove the camera from the body to clean it. Our device uses a continuously rotating sphere on the end of the laparoscope camera to continuously clean debris and provide unobstructed images, without interfering with surgery.
Noninvasive measuring of jugular vein pressure

Team Members: Connor Landgraf, Sneha Thatipelli, Sachin Rangarajan, Zhuchen Xu
Capstone Client: John Chorba, MD, Resident Physician at UCSF
Purpose: Measuring jugular venous pressure (JVP) is an indirect screening tool for the presence of heart disease, but the effectiveness of the current measurement technique varies from user to user. In order to accurately measure JVP in a user-independent manner, our group developed a probe that can detect the pressure required to momentarily collapse the jugular vein. The pressure read by this device outputs a clear signal to a display that can be read unambiguously by the user.
Measure pressure applied with a device designed to stem bleeding during childbirth
Team Members: Sandeep Prabhu, Atri Choksi, Alish Manandhar, Rebecca Farr
Capstone Client: Suellen Miller, PhD, CNM, Principal Investigator of the LifeWrap Project and Director of Safe Motherhood Program at UCSF; Elizabeth Butrick, MSW, MPH, LifeWrap project director at the Safe Motherhood Program at UCSF
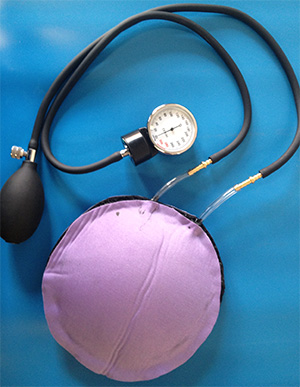
Purpose: Postpartum hemorrhage—excessive blood loss from the uterus after childbirth—is the leading cause of maternal mortality, particularly in the developing world. Hemorrhaging is most commonly caused when the uterus fails to contract after childbirth. The LifeWrap is a full-body tourniquet that helps to slow blood loss, contract the uterus, and direct blood towards vital organs to avoid hemorrhagic shock. The LifeWrap is not always effective, primarily due to variability in how much pressure is applied to patients. Our team developed a device that can interface with the LifeWrap to monitor the pressure applied to the patient’s uterus over time. We created a neoprene inflatable bladder with a pressure sensor that can be attached to the LifeWrap and is capable of both measuring the applied pressure and augmenting it via the inflatable bladder.
An emergency medical transport solution for developing countries

Team Members: Inbal Epstein, Tak Yau, Susanna Ly, Arthur King
Capstone Client: Rai Vohra, MD, Assistant Clinical Professor of Emergency Medicine at UCSF – Fresno
Purpose: Many developing countries lack both pre-hospital resources (e.g. ambulances) and the infrastructure for automobiles, making it difficult to administer healthcare to injured individuals. Our team worked to develop an adaptable patient transportation system which is low cost, durable and can traverse a variety of terrains for use in Haiti and Nepal. We developed a cart system with a removable stretcher and a flexible hitch to attach it to different transport methods like a bike, mule, or motorcycle. The system is designed to be built with readily available materials, such as bamboo and bicycle wheels.
Portable newborn health screening devices

Team Members: Olga Miakicheva, Michael Nasr, Devi Khoday. Hosna Akhlaghpour
Capstone Client: Lisa Thompson, RN, PhD, FNP-C, Assistant Professor in School of Nursing at UCSF
Purpose: The birth-weight and vital-signs of infants at birth are strong predictors of neonatal mortality. However, in resource-poor countries where the majority of births occur at home, health screening of infants is difficult and too costly. Our team developed devices for screening the health of home-delivered newborns that can be used by midwives of varying educational levels in Guatemala to ensure that medical abnormalities in neonates are promptly identified. We developed a hand-held device with a pictorial interface where midwives enter data measurements (e.g. skin color, level of movement), and the device outputs an overall health assessment. We designed an electronic version to train users and verify proper use, as well as a mechanical version for wide distribution in Guatemala.
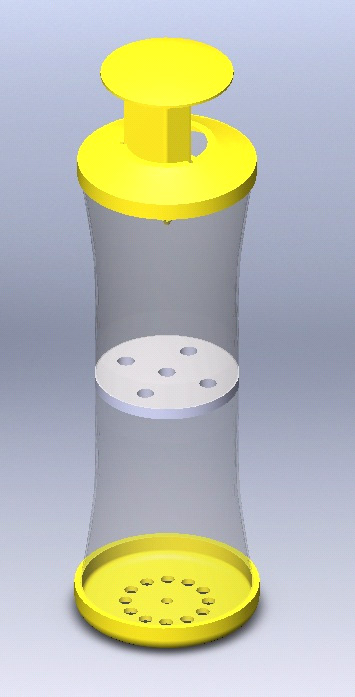
Reduce malaria transmission by killing mosquitos without insecticides
Team Members: Kellen Chen, Helen Wan, Richard Hwang
Capstone Client: Bryan Greenhouse, MD, Assistant Adjunct Professor at UCSF
Purpose:
Malaria is a mosquito-borne infectious disease transmitted to humans through mosquito bites. Millions are infected with malaria each year, and the majority of cases occur in underdeveloped countries in Africa such as Uganda. Insecticide-treated mosquito nets are an inexpensive way to reduce malaria transmission, but the increase of insecticide-resistant mosquitoes has reduced in efficacy of these nets. Our team designed an insecticide-free, durable, low-cost method to divert mosquitoes away from humans that could be used in Ugandan households to reduce the prevalence of malaria. Our device is a hanging trap that attracts mosquitoes using soiled clothing such as a dirty sock. This method uses a natural, renewable attractant that is supplied by the user, allowing it to be easily and cheaply deployed in developing countries.
