2014 Respiratory Assist Device for ALS
Client: Björn Oskarsson, MD, Assistant Professor of Clinical Neurology, Director of UC Davis Multidisciplinary ALS clinic, University of California Davis Medical Center
Team: Sabrina Levy, Chris Deeble, Sravani Kondapavulur, Sivan Marcus
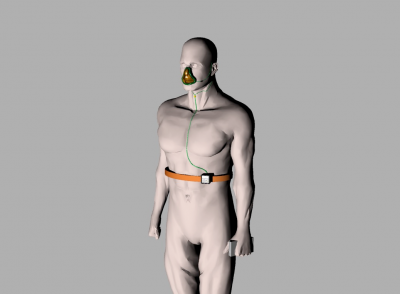
Purpose:
Amyotrophic Lateral Sclerosis (ALS), also known as “Lou Gehrig’s Disease”, affects around 30,000 Americans. The mean age of onset of ALS is 55, with 50% of patients dying within 3 years, and 75% within 5 years. Patients with ALS experience a gradual motor degeneration, during which they lose mobility throughout their body. The loss of diaphragm innervation necessitates the transition to respiratory assist devices as they lose the ability to breathe independently. Patients with relatively minimal loss of diaphragm control use a bilevel positive airway pressure (BiPAP) device intermittently, which ventilates through a mask over the face. Patient compliance with this device is low, as the BiPAP interferes significantly with their daily life. The next stage in respiratory assist devices is the installation of an invasive ventilator with a tracheostomy. As patients reach respiratory failure in the later stages of ALS, they lose the ability to speak. Due to the low quality-of-life and strong stigma associated with the invasive ventilator, many patients choose to die rather than undergo a tracheostomy. As the patient compliance with ventilation treatments significantly influences lifespan, design of a device that better encourages compliance is critical. This project seeks to develop a noninvasive respiratory assistance device that increases oxygenation while minimizing disturbances to daily life.


